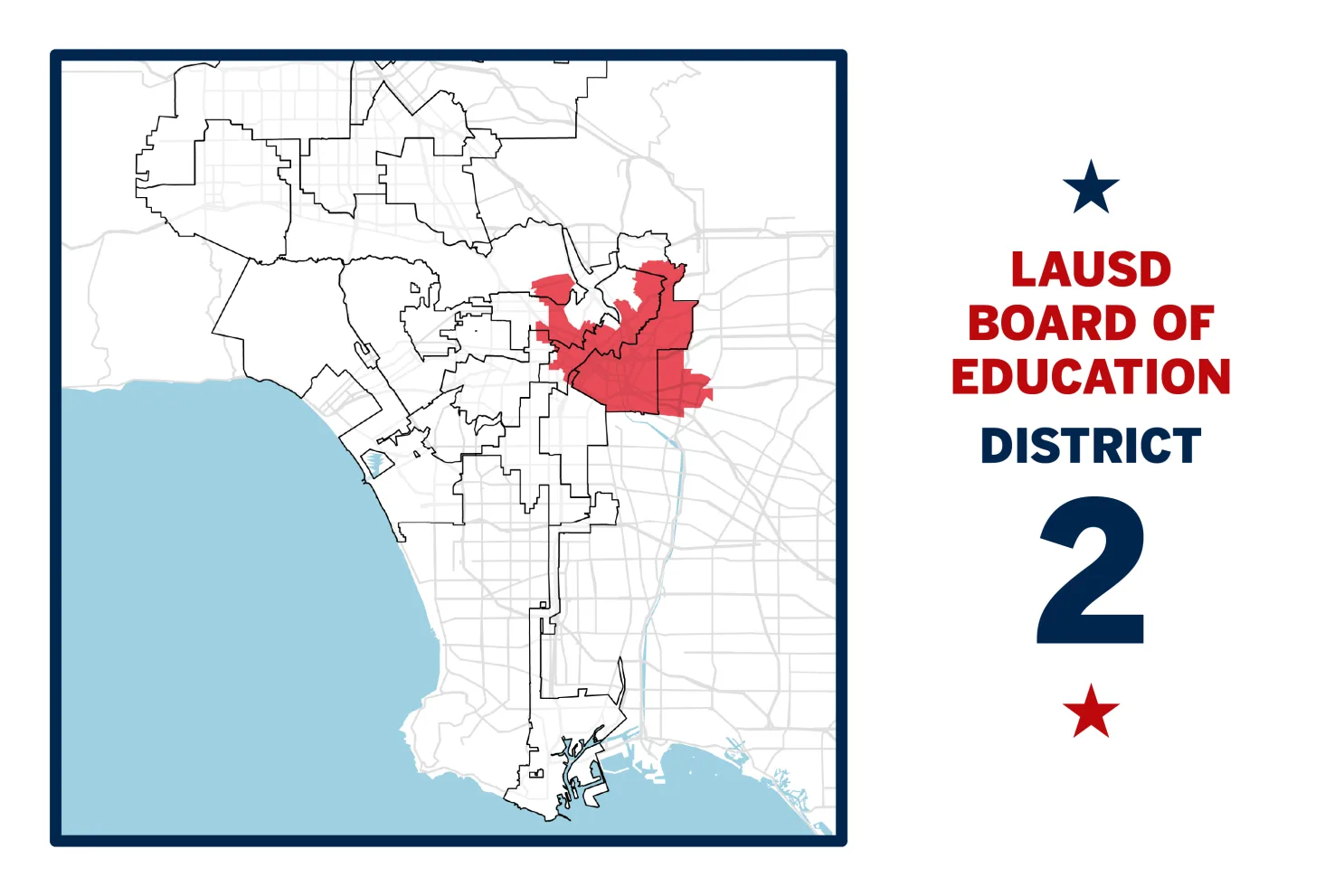
The 2026 Main Residency Match, the largest in the program's 74-year history, filled 41,482 positions from 48,050 active applicants. The outcome triggered calls on social media for new restrictions on international medical graduates, with critics claiming U.S. medical graduates had been squeezed out of training slots. Policymakers and public figures with large platforms have begun pursuing legislation to restrict visa sponsorship for internationally trained physicians. An examination of the actual match data, however, reveals no factual basis for these displacement claims.
U.S. medical school graduates posted strong match rates: 93.5% for M.D. graduates and 93.2% for D.O. graduates. These rates have remained stable between 92% and 95% since 1982, according to the American Medical Association. By contrast, the match rate for non-U.S. international medical graduates—physicians who are neither U.S. citizens nor permanent residents—stood at 56.4%, an all-time low despite a 52% surge in applications from this group between 2022 and 2026.
The residency system left 2,772 first-year positions unfilled across the country. Of these, 899 were in family medicine, 537 in internal medicine, 175 in pediatrics, and 65 in psychiatry. A total of 1,942 U.S. medical school seniors went unmatched. Even if every unmatched U.S. graduate had filled one of the open positions, approximately 800 slots would have remained empty. This surplus of vacancies contradicts the displacement narrative.
Specialty-level analysis shows that U.S. and international medical graduates are not competing for the same positions. In dermatology, internal medicine, thoracic surgery, and plastic surgery, U.S. M.D.s filled between 90% and 100% of available positions, while non-U.S. international medical graduates filled between zero and 3.6% in those same fields. International medical graduates concentrate in lower-paying specialties with high burnout rates: pediatrics, family medicine, and internal medicine.
Structural factors explain this pattern. U.S. medical school graduates carry an average debt of $200,000 and must pursue higher-paying specialties to manage loan repayment. A 2024 survey by the Association of American Medical Colleges found that 63% of graduating students planned to use loan-forgiveness programs, with 88% targeting the public service loan forgiveness program. The specialties where international medical graduates cluster—primary care fields—offer lower compensation and higher burnout, making them less attractive to debt-burdened U.S. graduates.
Program-level data further demonstrate structural separation. The top 15 pediatric residency programs with the highest international medical graduate representation are all community or community-university programs. The non-military pediatrics programs with the lowest international medical graduate representation are overwhelmingly university programs. Geographic practice patterns also diverge: international medical graduates disproportionately serve underserved, lower-income communities, often on J1 visas requiring work in medically underserved areas to satisfy home country requirements.
The underlying workforce challenge stems from policy decisions, not immigrant competition. Medicare graduate medical education reimbursement was capped at 1996 resident counts under the Balanced Budget Act of 1997, creating a structural barrier to training expansion even as U.S. medical school enrollment grew substantially. The nation faces a projected physician shortage of up to 86,000 by 2036, with primary care bearing a disproportionate share. The Resident Physician Shortage Reduction Act, which would add 14,000 Medicare-supported positions over seven years, has been introduced in Congress but has not received a vote.
Restricting international medical graduate participation would likely worsen shortages in the specialties and communities already underserved, according to the data analysis.